What is Arthritis?
At its core, arthritis involves the breakdown of the tissues that allow joints to move smoothly. In a healthy joint, cartilage acts as a slippery cushion between bones. In arthritis, this cartilage thins or the joint lining (synovium) becomes inflamed and swollen.
The most common types include:
-
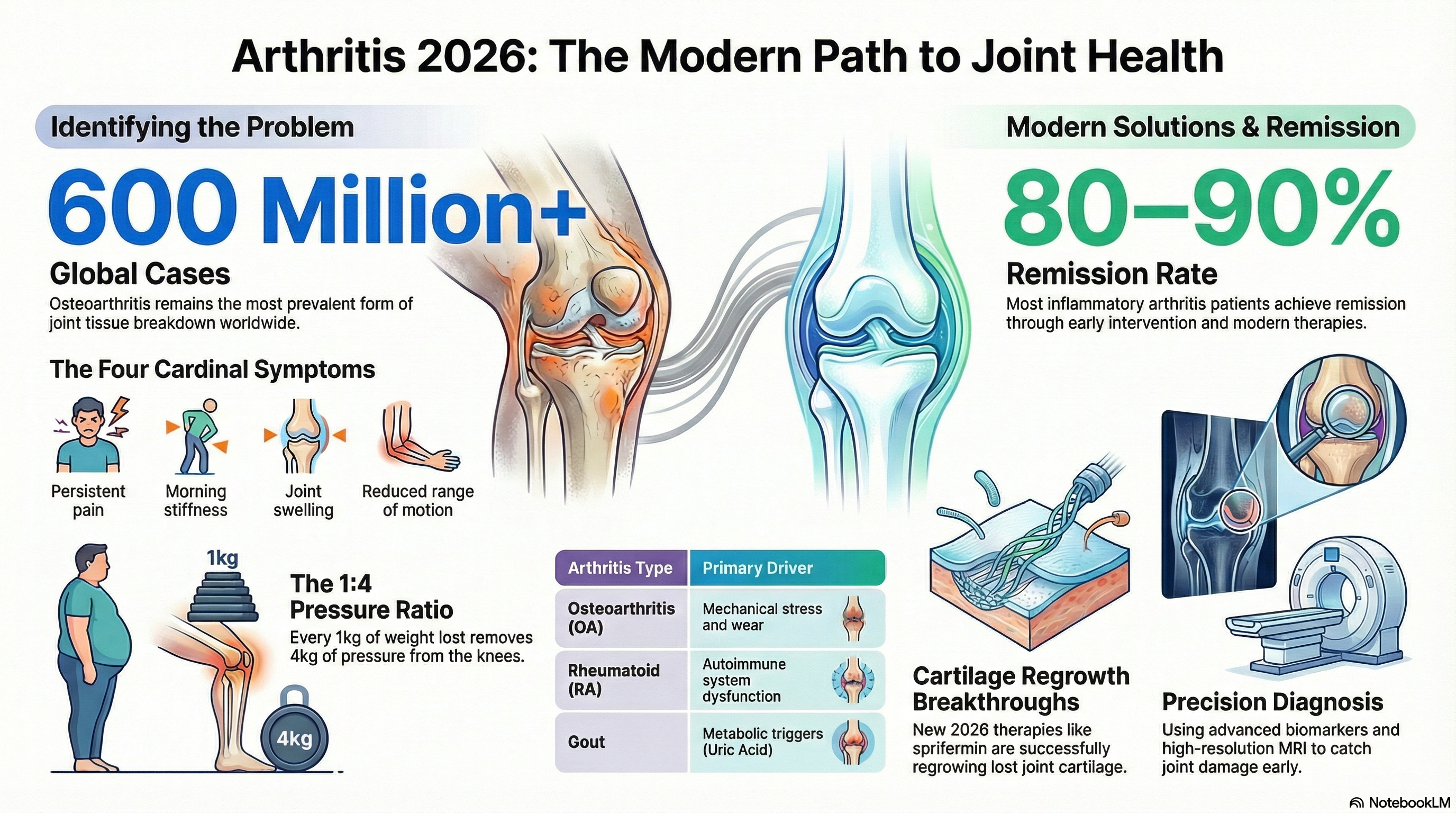
Osteoarthritis (OA): Often called "wear and tear" arthritis, it is the most prevalent form, affecting over 600 million people globally. It involves the gradual breakdown of cartilage.
-
Rheumatoid Arthritis (RA): An autoimmune disease where the immune system mistakenly attacks the joint lining.
-
Psoriatic Arthritis: A condition that affects some people who have the skin condition psoriasis.
-
Gout: A painful condition caused by the buildup of uric acid crystals in the joint, often starting in the big toe.
Causes of Arthritis
The cause of arthritis depends entirely on the specific type being diagnosed. The two primary mechanisms are mechanical breakdown and immune system dysfunction.
Mechanical Stress and Wear Osteoarthritis is primarily caused by the cumulative effects of age, obesity, and mechanical stress. Excessive weight puts significant pressure on weight-bearing joints like the knees and hips, while previous injuries can cause joints to wear out prematurely.
Autoimmune and Genetic Factors Inflammatory types like Rheumatoid Arthritis and Ankylosing Spondylitis are caused by an overactive immune system. Genetics play a major role; for example, the HLA-B27 gene is strongly linked to spinal arthritis.
Metabolic Triggers Gout is caused by "hyperuricemia"—too much uric acid in the blood. This can be triggered by a diet high in purines (red meat, shellfish, and alcohol) or by the body’s inability to process these substances efficiently.
Symptoms of Arthritis
While each type has unique features, almost all forms of arthritis share a set of cardinal symptoms that impact daily life.
-
Pain: This is the most common symptom. In "wear and tear" types, pain is usually provoked by activity. In inflammatory types, pain may actually be worse during rest.
-
Stiffness: Especially noticeable in the morning. For those with RA, morning stiffness may last for more than an hour.
-
Swelling and Warmth: Inflamed joints may look puffy and feel warm to the touch due to increased blood flow and fluid buildup.
-
Reduced Range of Motion: Difficulty fully bending or straightening a limb.
-
Fatigue: A deep, systemic exhaustion often accompanies the autoimmune forms of the disease.
-
Joint Deformity: In advanced stages, joints may shift out of alignment or develop visible lumps.
Diagnosis of Arthritis
Diagnosis has evolved into a precision process in 2026, utilizing advanced biomarkers and high-resolution imaging to catch the disease early.
Laboratory Testing Blood tests look for specific markers of inflammation (CRP and ESR) or antibodies that indicate an autoimmune response (Rheumatoid Factor and anti-CCP). For gout, doctors measure uric acid levels in the blood or analyze joint fluid for crystals.
Advanced Imaging
-
X-rays: Useful for seeing bone spurs and narrowed joint spaces in advanced osteoarthritis.
-
Ultrasound: A highly sensitive tool for detecting early-stage inflammation and fluid in the joints.
-
MRI: The gold standard for identifying early rheumatoid arthritis or spinal involvement that an X-ray might miss.
Treatment of Arthritis
The goal of modern treatment is to achieve "remission"—a state where there is little to no active inflammation—and to preserve joint function.
Medical Breakthroughs (2025–2026)
-
Biologics and JAK Inhibitors: These targeted therapies have revolutionized the treatment of RA and Psoriatic Arthritis, allowing many patients to live virtually symptom-free.
-
Cartilage Regrowth: New therapies, such as sprifermin, are showing success in Phase 3 trials for actually regrowing cartilage in OA patients.
-
Nerve Ablation: Procedures like cooled radiofrequency ablation provide dramatic, long-term pain relief for those with severe knee or hip pain who aren't ready for surgery.
Lifestyle and Physical Support
-
Exercise: Low-impact activities like swimming, Tai Chi, and cycling are "medicine" for the joints, reducing pain as effectively as some medications.
-
Weight Loss: Losing just 1 kg (about 2.2 lbs) of body weight removes 4 kg (nearly 9 lbs) of pressure from the knees.
-
Diet: The Mediterranean diet is clinically proven to reduce flares in inflammatory arthritis.
Prevention of Arthritis
While genetic factors cannot be changed, you can take proactive steps to prevent or delay the onset of joint damage.
Joint Protection Maintaining a healthy weight is the single most effective way to prevent osteoarthritis. Additionally, proper "joint mechanics"—using your body correctly during heavy lifting or sports—helps prevent the injuries that often lead to arthritis later in life.
Diet and Supplements
-
Anti-inflammatory Foods: Regular consumption of Omega-3 fatty acids (fish oil) and turmeric (curcumin) can help dampen the body's inflammatory response.
-
Gout Prevention: For those prone to gout, avoiding beer, red meat, and shellfish while staying hydrated is essential.
-
Early Intervention: Seeking medical advice at the first sign of persistent joint pain or morning stiffness is the best way to prevent permanent damage. With modern 2026 treatments, 80–90% of patients with inflammatory arthritis can achieve remission if they start treatment early.





