What is Heart Failure?
Heart failure is generally classified by how well the left ventricle—the heart's main pumping chamber—is functioning. This is measured by the Ejection Fraction (EF), which is the percentage of blood the heart pumps out with each beat.
-
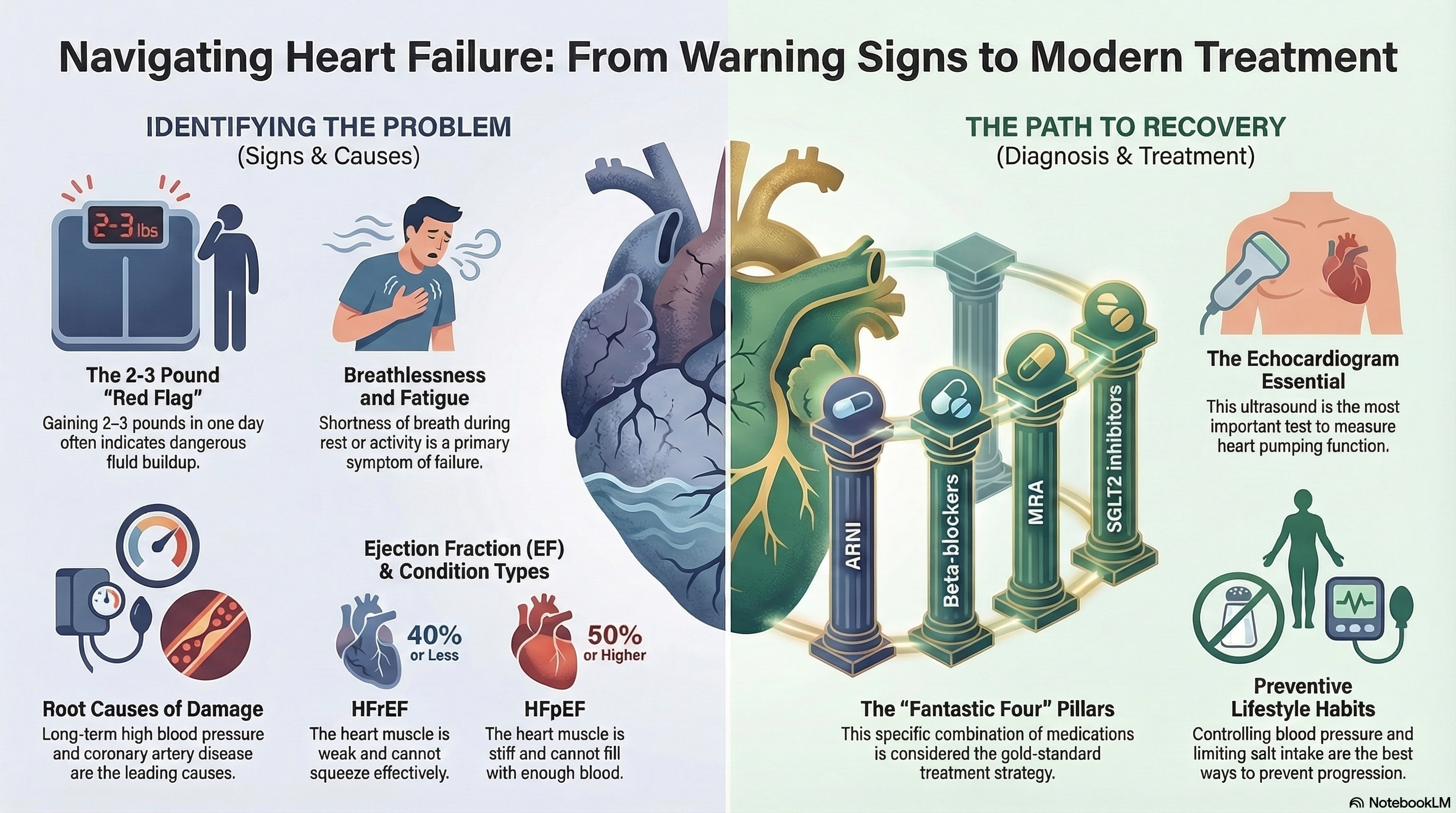
Heart Failure with Reduced Ejection Fraction (HFrEF): The heart muscle is weak and cannot squeeze effectively. The EF is typically 40% or less.
-
Heart Failure with Preserved Ejection Fraction (HFpEF): The heart muscle is stiff and cannot relax or fill with enough blood between beats. The EF remains at 50% or higher.
-
Heart Failure with Mildly Reduced Ejection Fraction (HFmrEF): The EF falls in the middle range of 41% to 49%.
Physicians also use a staging system (Stages A through D) to track the progression of the disease, moving from those "at risk" (Stage A) to those with "refractory" or end-stage heart failure (Stage D).
Causes of Heart Failure
Heart failure is usually the result of another condition that has damaged or overstretched the heart muscle over time.
-
Coronary Artery Disease: Blockages in the arteries can lead to heart attacks, which scar the heart muscle and weaken its pumping power.
-
High Blood Pressure (Hypertension): If blood pressure is high for a long time, the heart must work harder to circulate blood, eventually causing the muscle to become too stiff or too weak.
-
Heart Valve Disease: Malfunctioning valves force the heart to work harder to move blood in the right direction.
-
Cardiomyopathy: This is a general term for diseases of the heart muscle itself, which can be caused by genetics (up to 30% of cases), viral infections, heavy alcohol use, or certain chemotherapy treatments.
-
Abnormal Heart Rhythms: Conditions like Atrial Fibrillation (Afib) can cause the heart to beat too fast or irregularly, wearing out the muscle over time.
Symptoms of Heart Failure
The symptoms of heart failure occur because blood is backing up in the body and not enough oxygen-rich blood is reaching the organs and muscles.
-
Shortness of Breath (Dyspnea): Initially felt during exercise, but in advanced stages, it can occur while resting or lying flat (orthopnea).
-
Fatigue and Weakness: Feeling unusually tired during everyday activities like grocery shopping or climbing stairs.
-
Fluid Retention and Swelling (Edema): Swelling in the ankles, legs, or abdomen (ascites) caused by fluid backup.
-
Rapid Weight Gain: A sudden increase of 2–3 pounds in a single day or 5 pounds in a week is a major "red flag" for fluid buildup.
-
Persistent Cough: A dry cough or one that produces white or pink-tinged phlegm.
-
Paroxysmal Nocturnal Dyspnea: Waking up suddenly in the middle of the night gasping for air.
Diagnosis of Heart Failure
Early diagnosis is vital for improving long-term survival. Doctors use a combination of physical exams and specialized testing to confirm the condition.
-
Echocardiogram: This is the most important test. It uses ultrasound to create images of the heart, allowing the doctor to see how well it is pumping and measure the Ejection Fraction.
-
Natriuretic Peptide Tests (BNP or NT-proBNP): These are blood tests that measure a hormone that rises when the heart is under stress or stretched.
-
Electrocardiogram (ECG): To check for irregular heart rhythms or signs of a previous heart attack.
-
Chest X-ray: To see if the heart is enlarged or if there is fluid in the lungs.
-
Stress Tests or Coronary Evaluation: To determine if blocked arteries are contributing to the heart's weakness.
Treatment of Heart Failure
Modern medicine has revolutionized heart failure treatment. For patients with reduced ejection fraction (HFrEF), doctors now aim to prescribe the "Fantastic Four"—a combination of four classes of medicine proven to extend life and keep patients out of the hospital.
-
The Four Pillars:
-
ARNI (Entresto): A newer medication that replaces older ACE inhibitors or ARBs to improve heart function.
-
Beta-blockers: Medications like carvedilol or metoprolol that slow the heart rate and protect the heart from stress hormones.
-
MRA (Spironolactone): Helps prevent scarring of the heart tissue and manages fluid.
-
SGLT2 Inhibitors: Originally for diabetes, these drugs have shown a dramatic ability to reduce heart failure deaths even in people without diabetes.
-
-
Diuretics (Water Pills): Used to help the body flush out excess fluid and salt.
-
Devices: Some patients benefit from an ICD (to prevent sudden cardiac arrest) or CRT (a specialized biventricular pacemaker that helps the heart's chambers beat in sync).
-
Advanced Options: In end-stage cases, a Left Ventricular Assist Device (LVAD) or a heart transplant may be considered.
Prevention of Heart Failure
Preventing heart failure starts with managing the "Stage A" risk factors before any structural damage occurs to the heart.
-
Control Blood Pressure: Keeping blood pressure within a healthy range is the single most effective way to prevent heart failure, especially the "stiff heart" variety (HFpEF).
-
Manage Diabetes: High blood sugar damages blood vessels and heart tissue over time.
-
Maintain a Healthy Weight: Obesity increases the workload on the heart and is a major driver of heart failure risk.
-
Heart-Healthy Diet: Limit salt (sodium) intake to prevent fluid retention and focus on fruits, vegetables, and lean proteins.
-
Stay Active: Regular aerobic exercise strengthens the heart muscle and improves circulation.
-
Avoid Toxins: Limit alcohol consumption and do not smoke, as both directly damage heart cells and blood vessels.





