What is Hemorrhoids?
Hemorrhoids, also known as piles, are swollen, enlarged veins located in the anus and lower rectum, similar to varicose veins. They are an extremely common anorectal disorder, affecting approximately 1 in 2 adults by the age of 50.
Technically, everyone has "anal cushions"—vascular structures that normally help with stool control and sensation. We only refer to them as "hemorrhoids" when these cushions become abnormally enlarged, displaced, or inflamed. While they can be uncomfortable and alarming when they bleed, they are highly treatable and manageable with the right approach.
Causes of Hemorrhoids
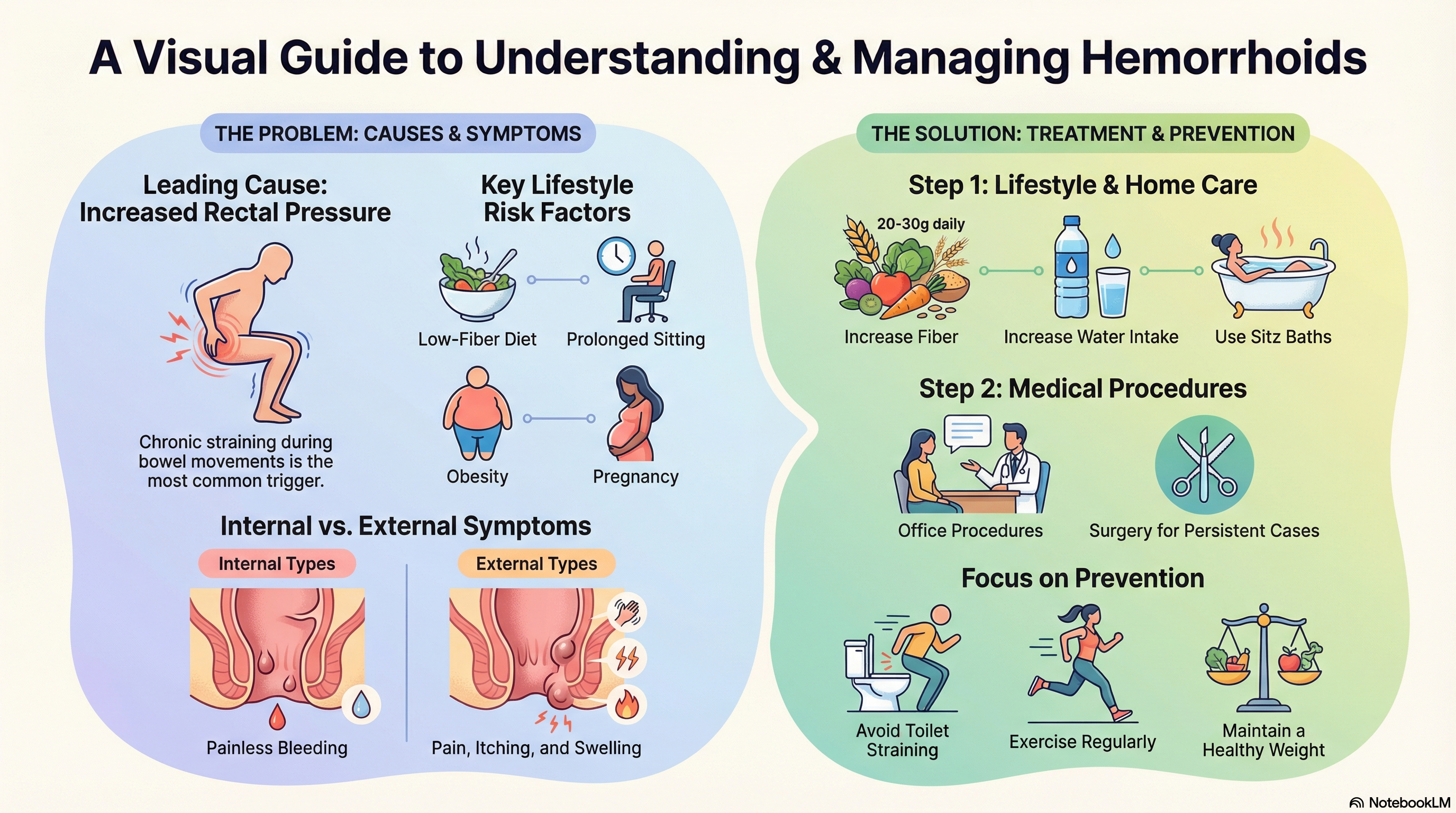
Hemorrhoids develop when there is increased pressure in the lower rectum or a weakening of the connective tissues that support the anal cushions. Common causes and risk factors include:
-
Chronic Straining: Pushing too hard during bowel movements is a leading cause.
-
Constipation or Diarrhea: Both conditions increase pressure and frequency of irritation to the anal canal.
-
Prolonged Sitting: Spending too much time on the toilet can cause blood to pool in the area, engorging the veins.
-
Pregnancy and Aging: Pregnancy increases abdominal pressure and causes hormonal changes, while aging naturally weakens the supporting tissues in the rectum.
-
Lifestyle Factors: A low-fiber diet, obesity, and heavy lifting can all contribute to the development of the condition.
-
Genetic Predisposition: A family history of hemorrhoids may make you more susceptible.
Symptoms of Hemorrhoids
Symptoms vary depending on whether the hemorrhoids are located inside or outside the anal opening.
-
Internal Hemorrhoids (Inside the rectum): These are usually painless because there are few pain-sensing nerves above the "dentate line." The most common sign is bright red blood on toilet tissue or in the bowl.
-
Prolapse: Internal hemorrhoids may push through the anal opening during a bowel movement. These are "graded" from I to IV based on whether they go back in on their own or need to be pushed back manually.
-
External Hemorrhoids (Around the anus): These can cause itching, irritation, or pain because the skin in this area is highly sensitive.
-
Thrombosis: If a blood clot forms in an external hemorrhoid, it becomes a Thrombosed Hemorrhoid, appearing as a hard, bluish-purple lump that causes sudden, severe pain.
Diagnosis of Hemorrhoids
Because rectal bleeding can also be a sign of more serious conditions like colorectal cancer or inflammatory bowel disease (IBD), a professional evaluation is essential.
-
Visual Inspection: A doctor examines the external area for swelling, skin tags, or prolapse.
-
Digital Rectal Exam (DRE): The physician inserts a lubricated, gloved finger into the rectum to feel for abnormalities or masses.
-
Anoscopy: A small, lighted tube (anoscope) is used to view the lining of the anus and lower rectum clearly.
-
Complete Endoscopic Evaluation: In some cases, especially for patients over 45 or those with specific risk factors, a colonoscopy or sigmoidoscopy may be recommended to rule out other causes of bleeding.
Treatment of Hemorrhoids
Treatment is typically "stepped," moving from lifestyle changes to office procedures, and finally surgery for severe cases.
-
Conservative Management: First-line treatments include a high-fiber diet (20–30g daily), increased water intake, and warm "sitz baths" to soothe the area.
-
Office-Based Procedures: For persistent internal hemorrhoids, doctors may use Rubber Band Ligation (RBL), where a small band is placed around the base to cut off blood flow, or Sclerotherapy, which uses a chemical injection to shrink the tissue.
-
Surgical Management: For Grade IV or very painful thrombosed hemorrhoids, surgery may be required. Options include a Hemorrhoidectomy (removal of the tissue) or Stapled Hemorrhoidopexy (lifting the tissue back into place), which generally offers a faster recovery.
Prevention of Hemorrhoids
Preventing hemorrhoids is largely focused on maintaining soft stools and reducing rectal pressure through healthy habits:
-
Don't Wait: Go to the bathroom as soon as you feel the urge. Delaying it can make stool harder and more difficult to pass.
-
Avoid "Toilet Reading": Limit your time on the toilet to avoid unnecessary pressure on the anal veins.
-
Increase Fiber and Fluids: Eat plenty of fruits, vegetables, and whole grains, and drink 6–8 glasses of water daily.
-
Exercise: Regular physical activity helps prevent constipation and reduces the pressure associated with prolonged sitting or standing.
-
Healthy Weight: Managing your weight can significantly reduce the physical pressure on your pelvic area.





