What is Bulimia Nervosa?
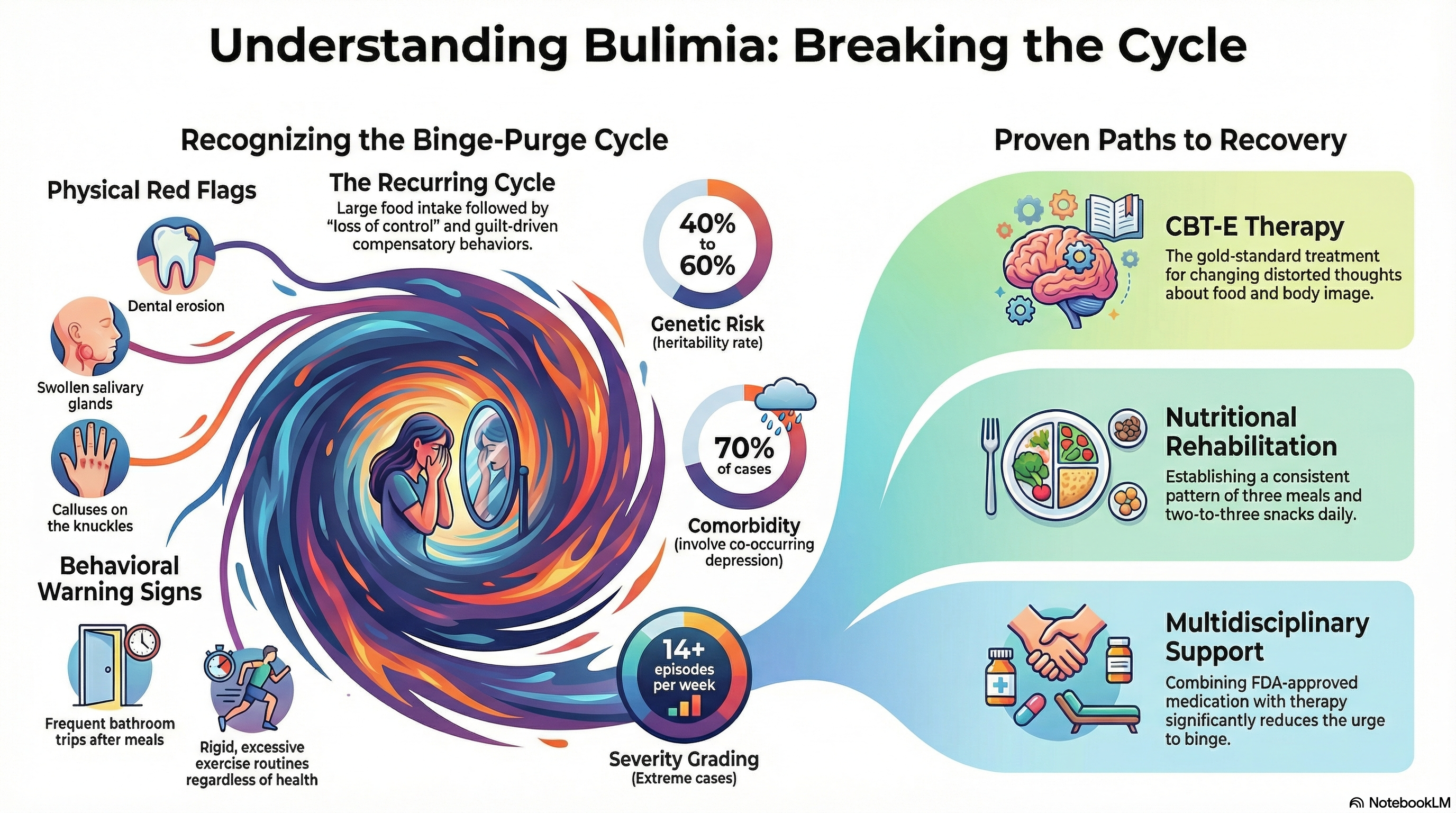
Bulimia is defined by two distinct behaviors that occur in a recurring cycle. First, a binge episode involves eating an amount of food in a short period (usually under two hours) that is significantly larger than what most people would consume. This is accompanied by a distressing sense of "loss of control."
Second, to manage the intense guilt or fear of weight gain following a binge, individuals engage in compensatory behaviors. These are categorized into two types:
-
Purging type: Self-induced vomiting or the misuse of laxatives, diuretics, or enemas.
-
Non-purging type: Using other methods such as excessive exercise (even when injured) or fasting for long periods.
For an official diagnosis, these behaviors must occur at least once a week for three months, and the person's self-worth must be excessively tied to their body shape and weight.
Causes of Bulimia Nervosa
There is no single cause for bulimia; rather, it results from a combination of biological, psychological, and environmental factors.
-
Genetic Factors: Bulimia has a high heritability rate of 40% to 60%. Having a family history of eating disorders or mood disorders significantly increases risk.
-
Neurobiology: Research indicates dysregulation in brain chemicals like serotonin and dopamine, which affect mood, impulse control, and the body's hunger signals.
-
Psychological Triggers: Traits like perfectionism, low self-esteem, and impulsivity are common. Many individuals use binging and purging as a way to cope with negative emotions or interpersonal stressors.
-
Sociocultural Pressures: Exposure to "thin-ideal" media and weight stigma can fuel body dissatisfaction.
-
Trauma: A history of childhood adversity or sexual abuse is a significant risk factor for many patients.
Symptoms of Bulimia Nervosa
Because many people with bulimia feel deep shame, they may go to great lengths to hide their symptoms. However, several physical and behavioral red flags often emerge over time.
Physical Signs
-
Dental Issues: Stomach acid from frequent vomiting erodes tooth enamel, leading to cavities, sensitivity, and discoloration.
-
Swollen Glands: Repeated vomiting can cause the salivary glands to swell, creating "chipmunk cheeks."
-
Russell’s Sign: Calluses or scars on the knuckles caused by using the fingers to induce vomiting.
-
Electrolyte Imbalance: Low levels of potassium or sodium can cause dehydration, heart palpitations, and dangerous heart arrhythmias.
Behavioral Signs
-
Disappearing to the bathroom immediately after meals.
-
Excessive use of mouthwash, mints, or gum to hide the smell of vomit.
-
Hiding large amounts of food wrappers or hoarding food.
-
Rigid exercise routines that are never missed, regardless of weather or health.
Diagnosis of Bulimia Nervosa
Diagnosis begins with a clinical interview by a doctor or mental health professional. Because bulimia often co-occurs with other conditions, a thorough assessment is vital.
-
Psychiatric Assessment: A professional will evaluate eating patterns, thoughts about body image, and the frequency of compensatory behaviors.
-
Physical Exam and Labs: Doctors will check for irregular heartbeats and order blood tests to look for electrolyte imbalances (especially potassium).
-
Severity Grading: The condition is graded based on the number of weekly episodes. Mild cases involve 1–3 episodes per week, while extreme cases involve 14 or more.
-
Screening for Comorbidities: Doctors also look for signs of depression (found in 70% of cases), anxiety, substance use disorders, or personality disorders.
Treatment of Bulimia Nervosa
Bulimia is highly treatable, and most people achieve full or partial recovery with a multidisciplinary approach.
-
Psychotherapy: Cognitive Behavioral Therapy (CBT-E) is the gold standard. It focuses on breaking the binge-purge cycle by changing distorted thoughts about food and body image. Interpersonal Psychotherapy (IPT) is also effective for addressing underlying relationship stressors.
-
Medication: Fluoxetine (Prozac) is currently the only FDA-approved medication specifically for bulimia. It can help reduce the urge to binge and purge, especially when combined with therapy.
-
Nutritional Rehabilitation: Working with a dietitian to establish a regular pattern of three meals and two to three snacks a day is essential to stop the "starve-binge" cycle.
-
Levels of Care: While most treatment is outpatient, intensive programs or hospitalization may be necessary if there are severe electrolyte imbalances or a high risk of self-harm.
Prevention of Bulimia Nervosa
While you cannot prevent a genetic predisposition, societal and personal shifts can help reduce the risk of developing the disorder.
-
Promoting Body Positivity: Challenging the "thin ideal" and focusing on what the body can do rather than how it looks.
-
Early Education: Teaching children and adolescents healthy ways to cope with emotions and stress can prevent them from turning to food as a coping mechanism.
-
Healthy Modeling: Encouraging regular, non-restrictive eating habits at home and avoiding "diet talk" or weight-shaming.
-
Early Intervention: Seeking help at the very first sign of disordered eating significantly improves the long-term prognosis. Recovery involves not just stopping the behaviors, but normalizing thoughts about food and weight.





