What is COPD?
COPD is an "umbrella" term that typically involves a combination of two distinct conditions:
-
Chronic Bronchitis: This involves long-term inflammation and narrowing of the bronchial tubes, which carry air to the lungs. It results in a persistent cough and excessive mucus production.
-
Emphysema: This occurs when the tiny air sacs (alveoli) at the end of the air passages are destroyed. This reduces the surface area of the lungs and makes it harder for oxygen to reach your bloodstream.
Unlike asthma, where airflow obstruction is often temporary and reversible, the obstruction in COPD is persistent and tends to worsen over time.
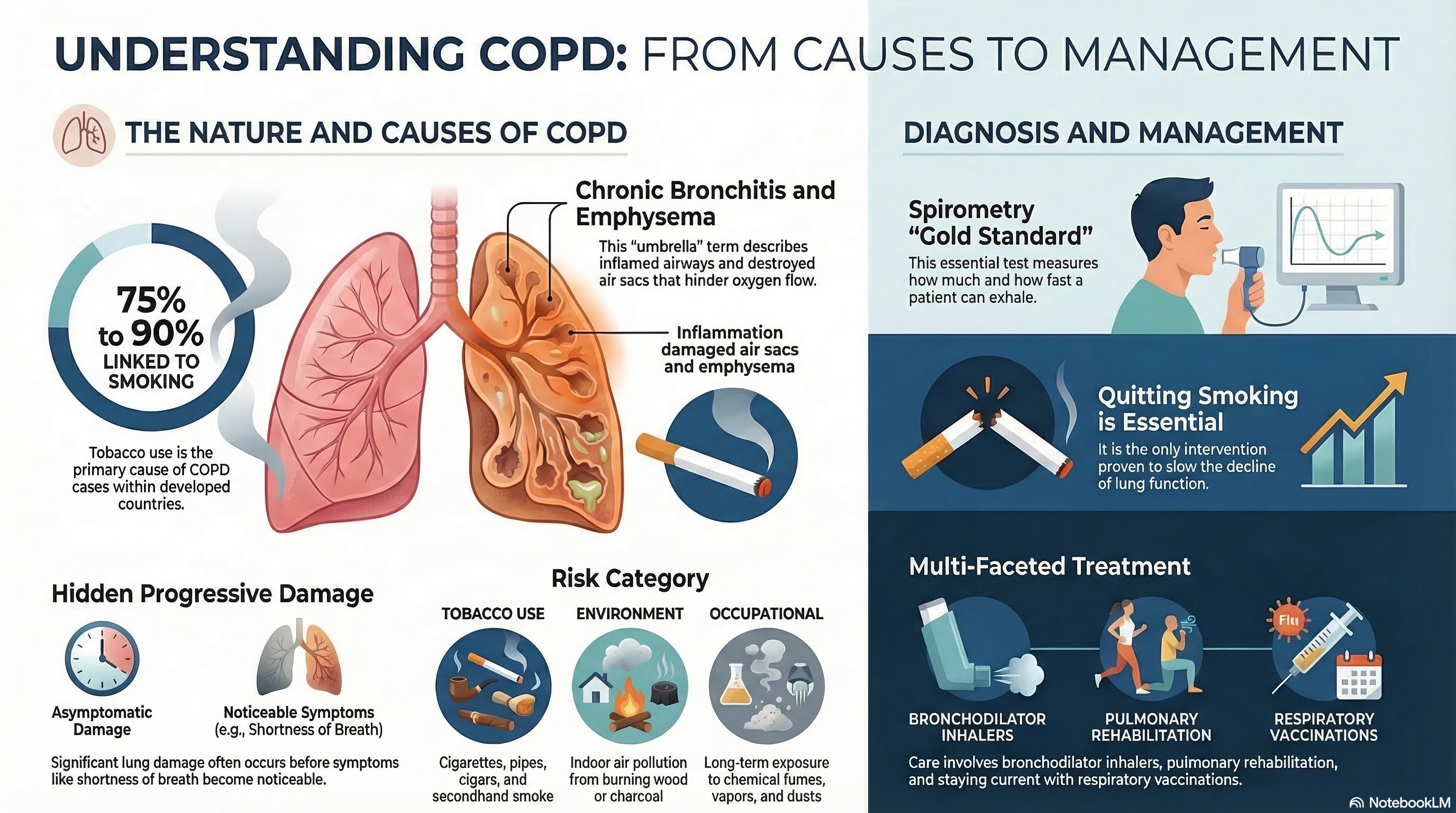
Causes of COPD
The primary cause of COPD is long-term exposure to irritating gases or particulate matter.
-
Smoking: Tobacco use is responsible for approximately 75% to 90% of cases in developed countries. This includes cigarettes, pipes, cigars, and secondhand smoke.
-
Environmental Exposures: In many parts of the world, indoor air pollution from burning wood or charcoal for cooking and heating (biomass fuel) is a leading cause, particularly among women.
-
Occupational Hazards: Long-term exposure to chemical fumes, vapors, and dusts in the workplace can damage the lungs.
-
Genetics: A rare genetic condition called Alpha-1 Antitrypsin Deficiency (AATD) can cause COPD in younger people, even those who have never smoked.
-
Early Life Factors: Premature birth, severe childhood respiratory infections, or poorly controlled asthma can increase the risk of developing COPD later in life.
Symptoms of COPD
Symptoms often do not appear until significant lung damage has occurred, and they usually worsen over time, especially if smoking continues.
-
Progressive Shortness of Breath (Dyspnea): Initially noticed during physical activity, but eventually occurring during rest.
-
Chronic Cough: Often referred to as "smoker's cough," this may produce significant amounts of mucus (sputum), especially in the morning.
-
Wheezing and Chest Tightness: A whistling sound when breathing or a feeling of pressure in the chest.
-
Frequent Respiratory Infections: Increased susceptibility to colds, the flu, or pneumonia.
-
Fatigue: A general lack of energy due to the extra effort required to breathe.
-
Advanced Signs: In later stages, patients may experience unintended weight loss, swelling in the ankles or legs, and a bluish tint to the lips or fingernails (cyanosis).
Diagnosis of COPD
If you have symptoms or a history of exposure to risk factors, your doctor will use specialized tests to confirm a diagnosis.
-
Spirometry: This is the gold standard for diagnosing COPD. You breathe into a machine that measures how much air you can exhale and how fast you can do it. A "post-bronchodilator" result showing limited airflow confirms the condition.
-
Imaging: A chest CT scan or X-ray can help identify emphysema, rule out other lung problems (like lung cancer), or assess the severity of airway thickening.
-
Assessment Tools: Doctors use standardized questionnaires like the CAT (COPD Assessment Test) or the mMRC scale to determine how much the disease affects your daily life.
-
Alpha-1 Testing: A simple blood test may be performed to check for the genetic form of the disease, especially in younger patients.
Treatment of COPD
While there is no cure, treatment focuses on relieving symptoms, improving quality of life, and preventing "exacerbations"—sudden flare-ups where symptoms get significantly worse.
-
Smoking Cessation: This is the single most important and effective step. It is the only intervention proven to slow the rate at which lung function declines.
-
Bronchodilators: These medications, usually taken through an inhaler, relax the muscles around your airways to make breathing easier. They include "LAMA" and "LABA" therapies.
-
Inhaled Corticosteroids (ICS): These may be added for patients who have frequent flare-ups or specific blood markers (high eosinophils).
-
Pulmonary Rehabilitation: This is a comprehensive program that includes exercise training, nutritional advice, and counseling. It is one of the most effective ways to improve your ability to stay active.
-
Oxygen Therapy: For patients with very low oxygen levels, supplemental oxygen can improve survival and quality of life.
-
Vaccinations: Staying up-to-date with flu, pneumonia, COVID-19, and Tdap vaccines is essential to prevent infections that can trigger dangerous flare-ups.
Prevention of COPD
Most cases of COPD are directly related to the air we breathe, making it a largely preventable disease.
-
Do Not Smoke or Quit Now: If you smoke, quitting is the most effective way to prevent the onset or progression of COPD.
-
Avoid Secondhand Smoke: Protect yourself and others by maintaining smoke-free environments.
-
Minimize Occupational Exposure: If you work around dust, fumes, or chemicals, use proper protective equipment and ensure the area is well-ventilated.
-
Reduce Indoor Air Pollution: Improve ventilation in the home, especially when cooking or using heating fuels.
-
Manage Respiratory Health: Treating asthma early and effectively can reduce the risk of it developing into a permanent obstruction like COPD.





