What is Cardiac Arrest?
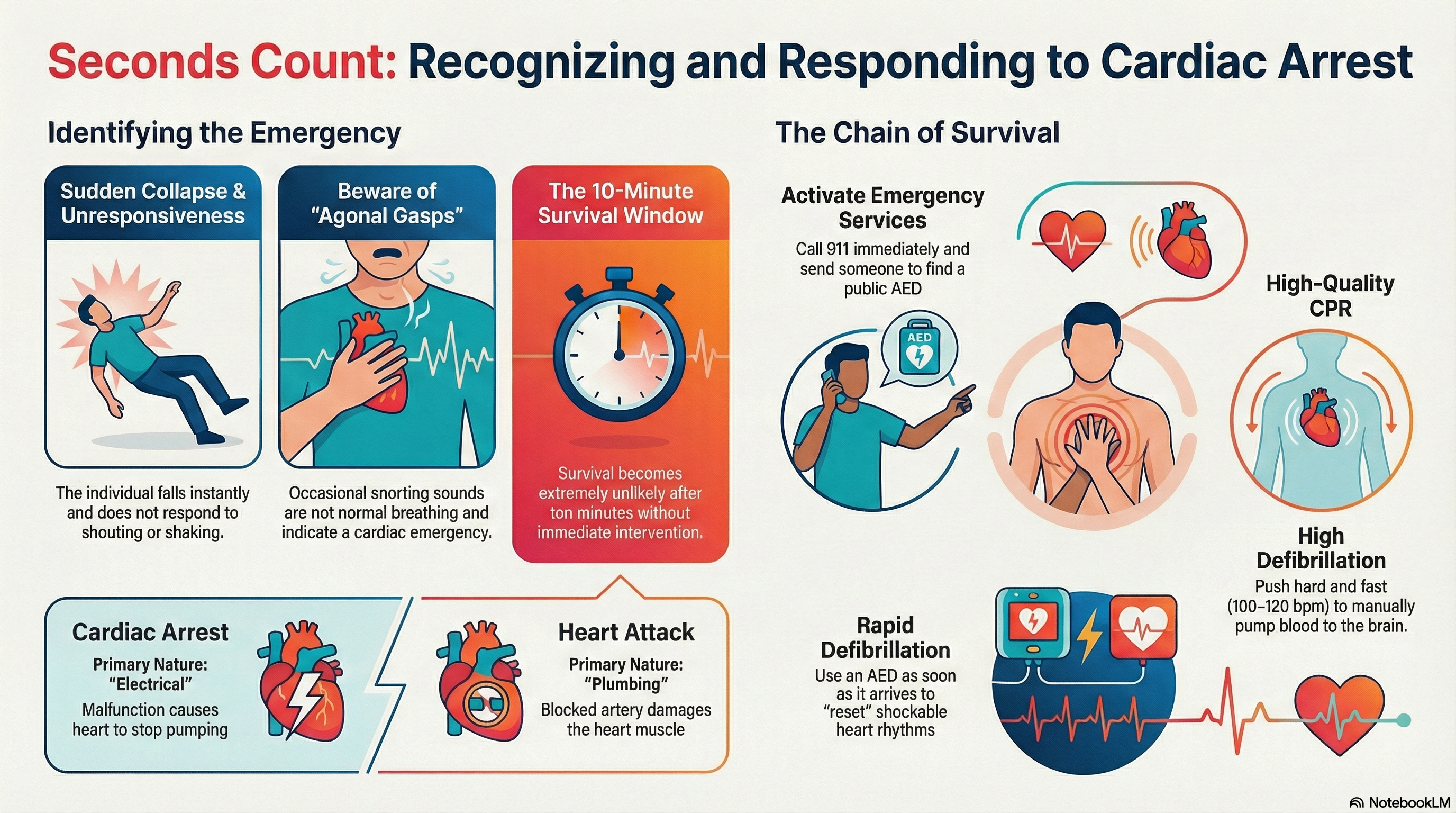
Cardiac arrest is often confused with a heart attack, but they are distinct conditions. A heart attack is a "plumbing" problem caused by a blocked artery that damages the heart muscle. Cardiac arrest is an "electrical" problem where a malfunction causes the heart to stop pumping blood to the rest of the body. While a heart attack can trigger cardiac arrest, many arrests occur due to other electrical or structural heart issues.
When the heart stops, blood flow to the brain and vital organs ceases instantly. Brain damage can begin in as little as four minutes, and survival becomes extremely unlikely after ten minutes without treatment.
Causes of Cardiac Arrest
The causes of cardiac arrest are generally divided into cardiac (heart-related) and non-cardiac categories.
Cardiac Causes (50-80% of cases)
-
Coronary Artery Disease: The most common cause in adults. Plaque buildup or a sudden blockage (heart attack) can disrupt the heart's electrical signals.
-
Cardiomyopathy: An enlarged or thickened heart muscle that is more prone to irregular rhythms.
-
Heart Valve Disease: Conditions like aortic stenosis can put excessive strain on the heart.
-
Inherited Rhythms (Channelopathies): Genetic conditions like Long QT Syndrome or Brugada Syndrome that affect the heart's electrical "wiring."
Non-Cardiac and Reversible Causes Emergency responders often use the "H's and T's" framework to identify reversible triggers:
-
H's: Hypoxia (lack of oxygen), Hypovolemia (severe blood/fluid loss), Hypo/Hyperkalemia (potassium imbalance), and Hypothermia.
-
T's: Toxins (such as opioid overdose), Tamponade (fluid around the heart), Tension Pneumothorax (collapsed lung), and Thromboembolism (pulmonary embolism).
Symptoms of Cardiac Arrest
Cardiac arrest usually happens with little to no warning. The primary signs are:
-
Sudden Collapse: The individual falls or slumps over instantly.
-
Unresponsiveness: They do not respond to shouting or shaking.
-
Abnormal Breathing: The person stops breathing entirely or may exhibit "agonal gasps"—occasional, labored snorting sounds that are often mistaken for normal breathing.
-
Loss of Pulse: There is no detectable heartbeat or pulse.
Diagnosis of Cardiac Arrest
Because every second counts, diagnosis is made based on simple clinical observations rather than complex tests.
-
Immediate Assessment: If a person is unresponsive and not breathing normally, they are assumed to be in cardiac arrest.
-
Heart Rhythm Analysis: Once an AED or professional monitor is attached, the "rhythm" is identified. Ventricular Fibrillation (VF) and Pulseless Ventricular Tachycardia (VT) are "shockable" rhythms where the heart is quivering and can be "reset" by a defibrillator. Asystole (flatline) and Pulseless Electrical Activity (PEA) are non-shockable rhythms that require high-quality CPR and medication.
-
Post-Resuscitation Testing: For survivors, doctors use EKG, echocardiograms, and coronary angiography to find the underlying trigger.
Treatment of Cardiac Arrest
Treatment follows a "Chain of Survival" that must be initiated immediately to be successful.
Immediate Emergency Steps
-
Recognition: Check for responsiveness and normal breathing.
-
Activation: Call 911 (or local emergency services) and send someone to find an AED.
-
High-Quality CPR: Start chest compressions (100–120 per minute, 5–6 cm deep) to manually pump blood to the brain.
-
Defibrillation: Use an AED as soon as it arrives. The device will voice-prompt you through the process and deliver a shock only if necessary.
Advanced Hospital Care
-
Medications: Epinephrine is used to help restart the heart; antiarrhythmics like Amiodarone are used for resistant rhythms.
-
Targeted Temperature Management: Cooling the body to approximately 36°C can help protect the brain from injury after the heart is restarted.
-
Implantable Cardioverter-Defibrillator (ICD): Most survivors receive an ICD, a small device placed under the skin that can automatically shock the heart back into rhythm if another arrest occurs.
Prevention of Cardiac Arrest
Prevention focuses on managing underlying heart health and preparing the community to respond.
-
Managing Heart Disease: Aggressive treatment of high blood pressure, high cholesterol, and diabetes reduces the risk of the coronary artery disease that leads to arrest.
-
Family Screening: If a close relative died suddenly before age 45, family members should undergo cardiac screening for inherited conditions.
-
Community Training: Widespread CPR training and public access to AEDs are the most effective ways to prevent death from out-of-hospital cardiac arrest.
-
Lifestyle Choices: Avoiding tobacco and illegal stimulants (like cocaine or amphetamines) and managing opioid prescriptions can prevent non-cardiac triggers.





