What is Cardiomyopathy?
There are five main types of cardiomyopathy, categorized by how the heart muscle changes:
-
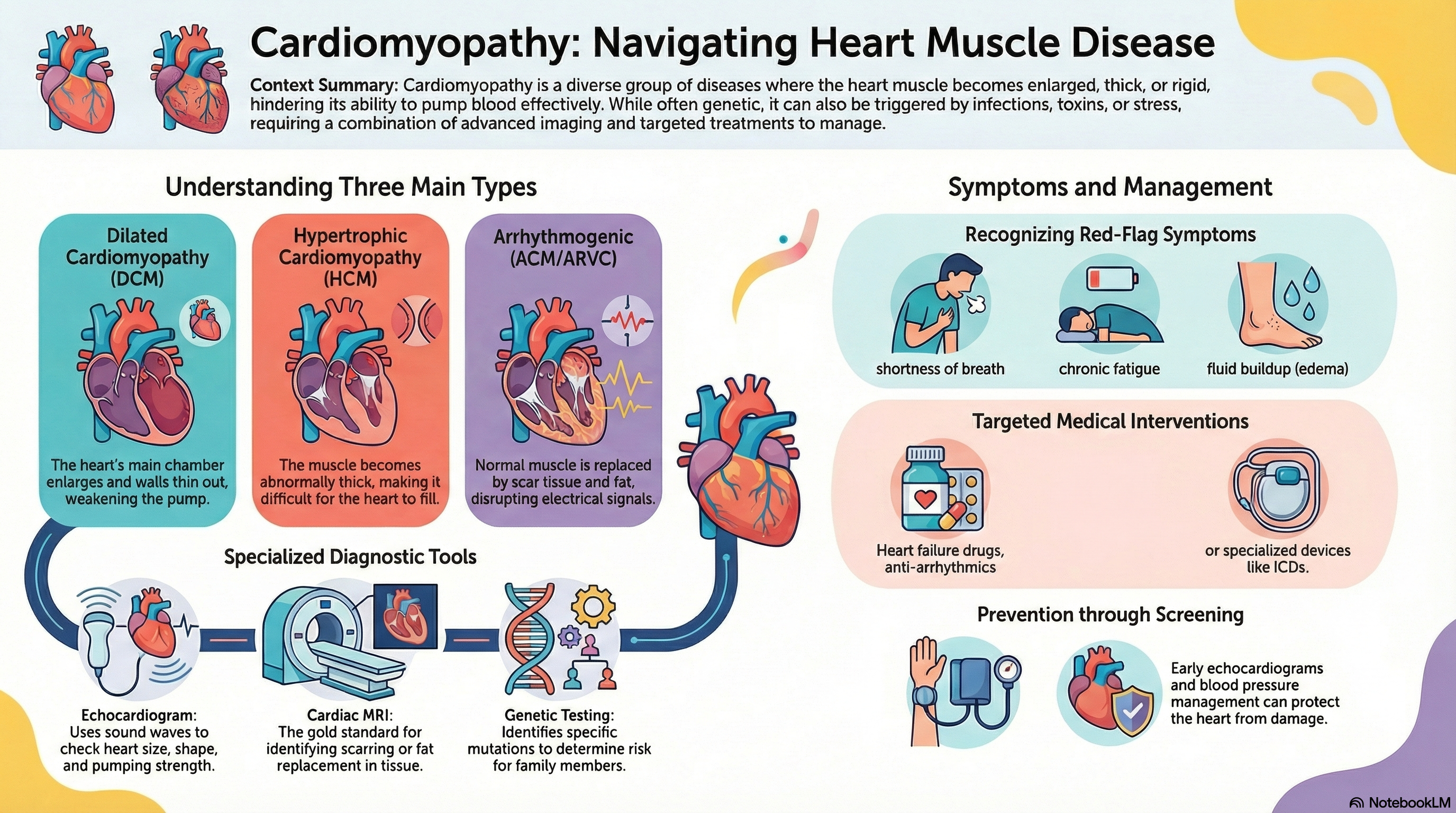
Dilated Cardiomyopathy (DCM): The most common type. The heart's main pumping chamber (the left ventricle) becomes enlarged (dilated) and the muscle walls thin out, weakening the heart's pump.
-
Hypertrophic Cardiomyopathy (HCM): The heart muscle becomes abnormally thick (hypertrophied), making it harder for the heart to fill with blood and pump it out. This is the most common primary genetic heart muscle disease.
-
Restrictive Cardiomyopathy (RCM): The heart muscle becomes stiff and rigid, meaning it cannot relax properly between beats to fill with blood.
-
Arrhythmogenic Cardiomyopathy (ACM/ARVC): Normal heart muscle is replaced by scar tissue and fat, which disrupts the heart's electrical signals and can cause life-threatening heart rhythms.
-
Takotsubo ("Broken Heart Syndrome"): A temporary weakening of the heart muscle, often triggered by extreme emotional or physical stress. It usually resolves within weeks.
Causes of Cardiomyopathy
Cardiomyopathy can be primary (starting in the heart itself, often due to genetics) or secondary (caused by another health condition or external factor).
-
Genetics: Many forms, especially HCM and ARVC, are inherited. If a close relative has the condition, genetic testing and family screening are often recommended.
-
Infections: Viral infections (myocarditis) can damage the heart muscle and lead to dilated cardiomyopathy.
-
Toxins: Long-term alcohol abuse, certain recreational drugs, and some chemotherapy medications can weaken the heart.
-
Pregnancy: A rare form called peripartum cardiomyopathy can develop during the final month of pregnancy or shortly after delivery.
-
Systemic Diseases: Conditions like amyloidosis (protein buildup), sarcoidosis (inflammation), or hemochromatosis (iron overload) can cause the heart muscle to become stiff or scarred.
Symptoms of Cardiomyopathy
In the early stages, many people have no symptoms. As the condition progresses, symptoms usually mimic those of heart failure:
-
Shortness of breath (Dyspnea): Especially during physical activity or when lying flat in bed.
-
Fatigue: Feeling unusually tired or exhausted during normal daily tasks.
-
Swelling (Edema): Fluid buildup in the ankles, legs, or abdomen.
-
Palpitations: A sensation of a racing, fluttering, or skipping heartbeat.
-
Dizziness or Fainting (Syncope): This can be a sign of a dangerous heart rhythm, especially in the hypertrophic or arrhythmogenic types.
Diagnosis of Cardiomyopathy
Because symptoms often overlap with other conditions, doctors use several specialized tests to confirm a diagnosis:
-
Echocardiogram: The most common tool. It uses sound waves (ultrasound) to create images of the heart's size, shape, and pumping strength.
-
Electrocardiogram (ECG/EKG): Records the electrical activity of the heart to look for signs of thickness or irregular rhythms.
-
Cardiac MRI: The "gold standard" for looking at the heart tissue itself, helping doctors identify scarring or fat replacement.
-
Blood Tests: To check for markers of heart stress (BNP) or to look for underlying causes like iron overload or thyroid issues.
-
Genetic Testing: Increasingly used to identify specific mutations that might put family members at risk.
Treatment of Cardiomyopathy
Treatment aims to manage symptoms, prevent the condition from getting worse, and reduce the risk of sudden complications.
-
Lifestyle Adjustments: Reducing salt intake to manage fluid buildup, limiting alcohol, and staying active within the limits set by your cardiologist.
-
Medications:
-
Heart Failure Drugs: ACE inhibitors, Beta-blockers, and SGLT2 inhibitors help the heart pump more efficiently and reduce the workload on the muscle.
-
Anti-arrhythmics: To control irregular heartbeats.
-
New Targeted Drugs: For example, mavacamten is a revolutionary new drug specifically for certain types of hypertrophic cardiomyopathy.
-
-
Implantable Devices:
-
ICD (Implantable Cardioverter-Defibrillator): A small device placed in the chest that can "shock" the heart back into a normal rhythm if it detects a life-threatening arrhythmia.
-
Pacemakers: To help the heart beat at a steady rate.
-
-
Surgery: In severe cases of HCM, a surgeon may remove part of the thickened muscle (myectomy). In end-stage cases of dilated cardiomyopathy, a heart transplant may be necessary.
Prevention of Cardiomyopathy
While you cannot prevent inherited (genetic) forms of the disease, you can take steps to protect your heart muscle from acquired damage.
-
Manage Blood Pressure: Keeping blood pressure in a healthy range reduces the long-term strain on the heart muscle.
-
Limit Alcohol and Toxins: Avoiding excessive alcohol and illegal stimulants can prevent toxic damage to the heart cells.
-
Early Screening: If you have a family history of sudden cardiac death or known cardiomyopathy, early screening with an echocardiogram can catch the condition before symptoms start.
-
Infection Control: Seeking prompt treatment for viral illnesses and staying up to date on vaccinations can reduce the risk of heart inflammation (myocarditis).





