What is Cellulitis?
Cellulitis occurs when bacteria penetrate the skin's protective outer layer and begin to multiply in the deeper tissues. This triggers a robust inflammatory response as the body tries to fight the "invaders."
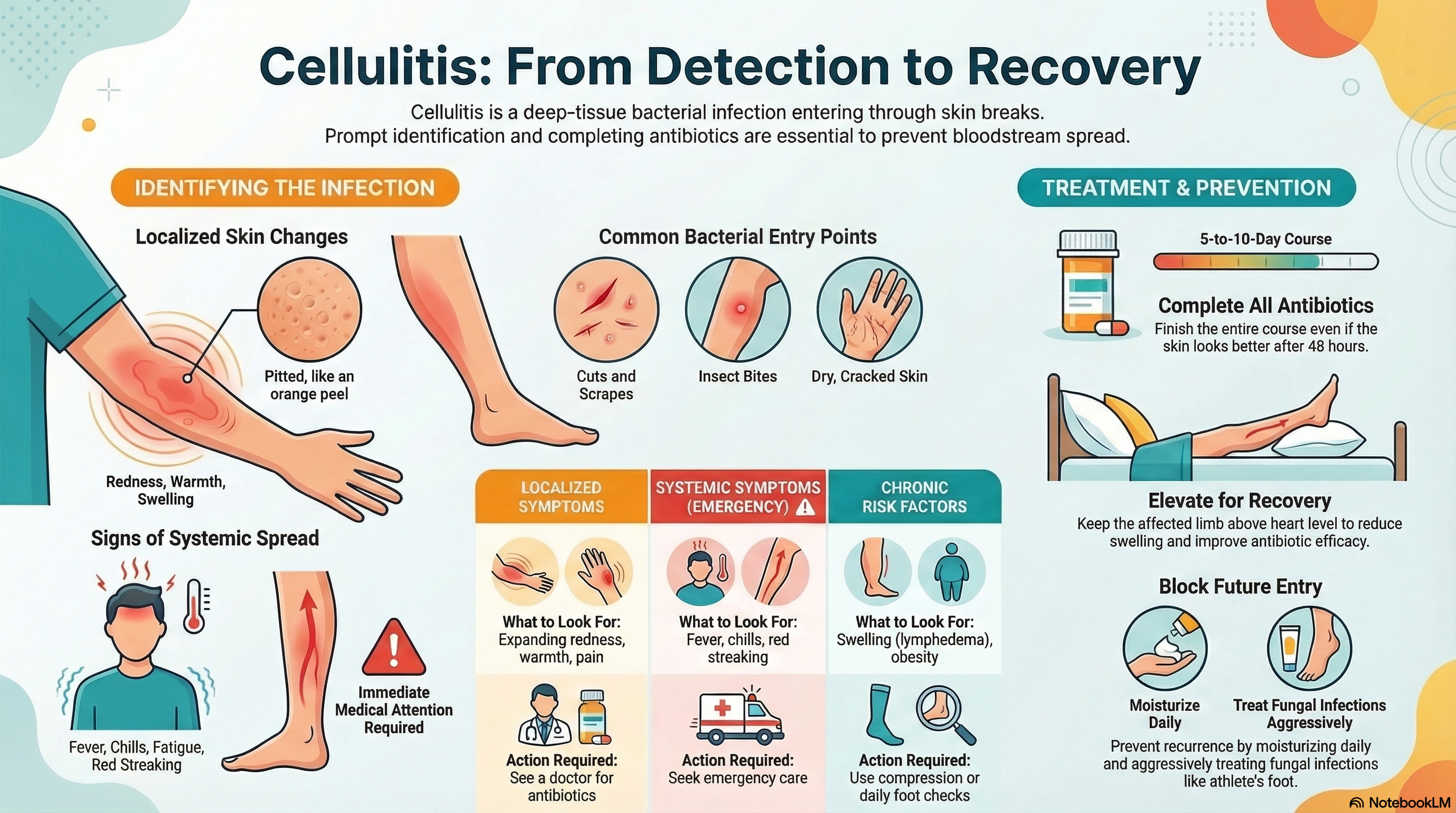
Because the infection is deep within the skin, the surface may not show an obvious open wound or pocket of pus initially. Instead, the area becomes red, swollen, and painful. If left untreated, the infection can spread to the lymph nodes and the bloodstream, which can become life-threatening.
Causes of Cellulitis
The infection is primarily caused by two types of bacteria: Streptococcus (Strep) and Staphylococcus (Staph). A specific type called MRSA (methicillin-resistant S. aureus) may be the cause in certain high-risk groups or regions.
Common Entry Points Bacteria need a "break" in the skin barrier to enter the body. Common entry points include:
-
Cuts, scrapes, or surgical wounds.
-
Insect bites or stings.
-
Athlete’s foot (tinea pedis): Fungal infections between the toes create tiny cracks that act as "doorways" for bacteria.
-
Chronic skin conditions like eczema or psoriasis.
-
Dry, cracked skin or ulcers caused by poor circulation.
Risk Factors You are at a higher risk for cellulitis if you have:
-
Chronic Swelling: Conditions like lymphedema or venous insufficiency that cause fluid to pool in the legs.
-
Weakened Immune System: Due to diabetes, chemotherapy, or certain medications.
-
Obesity: Which can impair circulation and lymphatic drainage.
-
History of Cellulitis: Once you have had it, you are more likely to experience a recurrence.
Symptoms of Cellulitis
Cellulitis symptoms usually appear on one side of the body and can spread rapidly.
Local Signs on the Skin:
-
A red area of skin that tends to expand.
-
The area feels warm or hot to the touch.
-
Swelling and tenderness or pain in the affected area.
-
Skin that appears "pitted" like an orange peel, or looks shiny and stretched.
-
Blisters or small spots may develop on top of the red skin.
Systemic Symptoms (Signs the infection is spreading):
-
Fever and chills.
-
Fatigue or a general feeling of being unwell (malaise).
-
Red "streaking" (lymphangitis) extending away from the original site of infection.
-
Swollen, tender lymph nodes near the area.
Diagnosis of Cellulitis
Diagnosis is primarily clinical, meaning a doctor can usually identify it just by looking at your skin and hearing your history.
-
Physical Exam: The doctor will check for warmth, redness, and swelling. They may mark the border of the redness with a pen to see if it continues to expand over the next 24 hours.
-
Medical History: Your doctor will look for potential entry points, like a recent scratch or a fungal infection between your toes.
-
Laboratory Tests: These are generally only needed for severe or recurring cases and may include blood tests to check for high white blood cell counts or "blood cultures" to see if the bacteria have entered your bloodstream.
-
Imaging: An ultrasound may be ordered if the doctor suspects a blood clot (DVT) or a hidden pocket of pus (abscess) under the skin.
Treatment of Cellulitis
The primary treatment for cellulitis is a course of antibiotics.
-
Oral Antibiotics: For mild cases, a 5-to-10-day course of oral pills (such as cephalexin or clindamycin) is standard. It is crucial to finish the entire prescription, even if your symptoms improve after a day or two.
-
IV Antibiotics: If the infection is severe, accompanied by a high fever, or not responding to pills, you may require intravenous (IV) antibiotics in a hospital setting.
-
Elevation: Keeping the affected limb elevated above the level of your heart is essential. This reduces swelling and helps the antibiotics work more effectively.
-
Pain Management: Over-the-counter pain relievers like acetaminophen or ibuprofen can help manage discomfort.
Note on Improvement: You should see an improvement within 48 to 72 hours of starting antibiotics. If the redness continues to spread rapidly or you develop a high fever, seek emergency care immediately.
Prevention of Cellulitis
Since up to 50% of people who have had cellulitis will experience it again, long-term prevention is a priority.
-
Skin Care: Keep your skin clean and moisturized to prevent cracks and dryness.
-
Treat Fungal Infections: Aggressively treat athlete’s foot or nail fungus, as these are common "hidden" entry points for bacteria.
-
Wound Care: Wash cuts or scrapes daily with soap and water, apply a protective ointment, and cover them with a bandage until they heal.
-
Manage Swelling: If you have chronic leg swelling, wearing compression stockings (as advised by your doctor) can significantly reduce your risk of infection.
-
Foot Inspections: If you have diabetes, check your feet daily for small injuries or blisters that you might not feel.
-
Prophylactic Antibiotics: In rare cases of frequent, repeated infections, a doctor may prescribe a low-dose daily antibiotic to prevent future episodes.





